Healing Leg Ulcers with Light Therapy
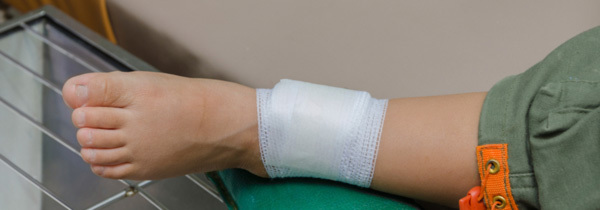
Leg ulcers are fairly common in elderly people with injuries to the leg. This condition simply entails a break in the skin of the leg, allowing air and bacteria to enter the underlying tissue. This type of injury normally heals up without any complications within a week or two. In some cases, however, there may be a biological problem (e.g., venous disease, arterial disease, diabetes or rheumatoid arthritis) that impedes the skin’s ability to heal, and this enables the affected area to increase in size, resulting in a chronic leg ulcer.
About 80% of these leg ulcers involve a dysfunction in the valves of veins that transport blood. A major consequence of this dysfunction is very high pressure in those same leg veins when the individual stands up. This abnormally high venous pressure poses a physical stress on the tissues, ultimately damaging the skin. In this way, chronic problems in the veins of the leg can result in chronic leg ulcers.
Treatment of a venous leg ulcer may involve elevation of the limb as well as compression bandaging or stockings to help keep the pressure in the leg veins at the ankle low when you are standing up. A number of different dressings may be used under the bandages depending on the state of the ulcer itself. For large or very resistant ulcers, either a skin graft or an operation on the veins may be needed. Many ulcers may take a fairly long time to heal, with most venous ulcers requiring several months, and a small proportion requiring even more time.
Photodynamic therapy, or PDT, has recently been proposed as a novel antimicrobial treatment that could help mitigate and circumvent the problem of antibiotic resistance. PDT has been highly effective in killing a broad spectrum of bacteria in cell culture studies.
Last year, researchers at the University of Dundee (United Kingdom) set up a controlled clinical study to determine if PDT in bacterially colonized chronic leg ulcers and chronic diabetic foot ulcers could reduce the bacterial load and speed up the wound healing process. The Dundee researchers enrolled 16 patients with chronic leg ulcers and 16 patients with diabetic foot ulcers, then randomly assigned half of each group to either a photosensitizer or a placebo.
Both groups were exposed to red light treatment, and the wound area was then carefully assessed up to three months following treatment. In contrast to the placebo, patients getting PDT showed a reduction in bacterial load immediately after treatment. After three months, 50% of patients with PDT-treated chronic leg ulcers showed complete healing, compared with only 12% of patients getting the placebo, as reported in the prestigious British Journal of Dermatology.
More recently, researchers at the Maria Nuova Hospital in Florence, Italy, conducted a pilot study in order to assess the variations of some parameters in chronic leg ulcers. The study included 15 patients who had not responded well to conventional treatments. These patients were then treated with PDT. The therapy was shown to increase the number and functionality of fibroblasts and to increase the clustering of mast cells with fibroblasts around blood vessels.
The researchers suggested that this could be the underlying mechanism by which PDT stimulates the formation of new blood vessels and bolsters the healing process following a leg ulcer, as reported ahead-of-print in the 13 June 2014 issue of Giornale Italiano di Dermatologia e Venereologia.
In another recent clinical trial, researchers at Azienda Ospedaliera Universitaria Careggi in Florence, Italy, sought to assess the antimicrobial effects and tolerability of PDT for infected foot ulcers in people with diabetes. This was a randomized, double-blind, placebo-controlled trial used PDT as an addition to antibiotic treatment with amoxicillin and clavulanic acid. The participants included 62 diabetic patients at least 18 years of age who had been diagnosed with an infected foot ulcer.
The Florence investigators observed a reduction in total bacterial load immediately after the light treatment, and this reduction was proportionate to the dose adminstered. The study’s conclusion, as reported in the June 2014 issue of the medical journal, Acta Diabetologia, was that PDT for infected diabetic foot ulcers is well tolerated and produces a significant reduction in the bacterial load.
Many infectious diseases continue to pose a serious public health threat around the world, and this threat is intensifying as antibiotic resistance continues to spread. Reasonable and effective alternatives are needed that are not susceptible to the problem of treatment resistance. PDT’s ability to eliminate light-sensitized bacteria could ultimately emerge as such an option, though larger clinical trials will be needed to better test its therapeutic potential for the treatment and management of chronic wounds.
Support us by buying our book, The Medicine of Light, and ebooks from our Photoimmune Discoveries eBook Series.
Sources
Corsi A, Lecci PP, Bacci S, Cappugi P, Pimpinelli N. Early activation of fibroblasts during PDT treatment in leg ulcers. G Ital Dermatol Venereol. 2014 Jun 13.[Epub ahead of print]
Morley S, Griffiths J, Philips G, Moseley H, O’Grady C, Mellish K, Lankester CL, Faris B, Young RJ, Brown SB, Rhodes LE. Phase IIa randomized, placebo-controlled study of antimicrobial photodynamic therapy in bacterially colonized, chronic leg ulcers and diabetic foot ulcers: a new approach to antimicrobial therapy. Br J Dermatol. 2013 Mar;168(3):617-24.
Wulf HC1, Karlsmark T. Photodynamic therapy of infected ulcers. Br J Dermatol. 2013 Mar;168(3):466. Mannucci E, Genovese S, Monami M, Navalesi G, Dotta F, Anichini R, Romagnoli F, Gensini G. Photodynamic topical antimicrobial therapy for infected foot ulcers in patients with diabetes: a randomized, double-blind, placebo-controlled study–the D.A.N.T.E (Diabetic ulcer Antimicrobial New Topical treatment Evaluation) study. Acta Diabetol. 2014 Jun;51(3):435-40.
© Copyright 2014, Photoimmune Discoveries, BV