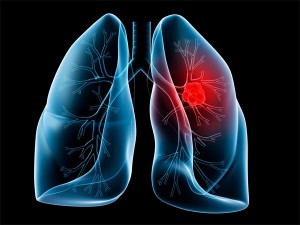
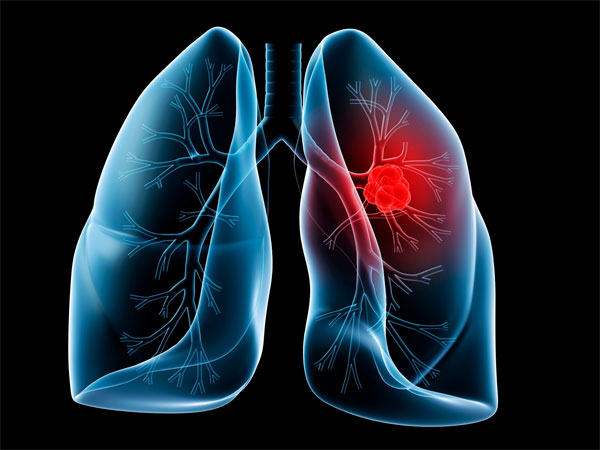
Tackling Lung Cancer the Photodynamic Way
Many tumors are first detected only after they’ve become bothersome or symptomatic. In the case of lung cancer, this usually means that the diagnosis takes place at a more advanced stage of the disease. With early detection, the disease can be treated more effectively, and long-range survival is far more likely.
This is why the approach called photodiagnosis, or photodynamic diagnosis, seems to hold such promise. Photodiagnosis entails the use of uses photosensitizers that selectively concentrate in cancerous tissue and fluoresce or “glow” when exposed to specific wavelengths of light.
The power of photodiagnosis is that it enables the physician to literally see where the abnormal tissue is. This method can detect even very tiny tumors as well as clusters of cancer cells that have not yet grown into a visible mass.
Catching cancer in its earliest phases of evolution, well before it has a chance to become malignant, helps set the stage for curative treatment.
Keys to Successful Photodynamic Therapy
Photodynamic therapy (PDT), is often a great choice for these early-stage situations, and it works as a logical complement to photo diagnosis. PDT uses a tumor-specific photosensitizer and low-power laser irradiation. In Japan and several other countries, PDT is now considered to be the first treatment of choice for central early-stage lung cancer.
Researchers at the Department of Thoracic Surgery, Nippon Medical School in Tokyo (Japan), recently studied the use of photodiagnosis for central lung cancer, a disease that affects the bronchi or central airways of the lungs. This form of lung cancer has responded extremely well to PDT.
To obtain a complete response with PDT, however, the Tokyo researchers emphasize that one must know how much cancer is in the bronchial mucosa and the depth of invasion to the bronchial wall. To this end, they espouse the use of a photodynamic diagnosis system using autofluorescence bronchoscopy (AFB) and a photosensitizer, which helps lower the risk of local recurrence after PDT.
Writing in the December 2013 Journal of Nippon Medical School, they describe the overall approach as follows: “Just before PDT, we perform photodynamic diagnosis with a AFB equipped with a diode laser (408 nm) to excite the photosensitizer and capture the red fluorescence emitted from the tumor; in this way we can accurately define the tumor margins. Immediately after PDT, photodynamic diagnosis is again performed to confirm the loss of red fluorescence emitted from the tumor, and a sufficient dose of laser illumination is given.”
The Tokyo research team explains that this procedure enables one to confirm that all the photosensitizer in the tumor had been “excited” by laser irradiation (664 nm), resulting in a loss of the red fluorescence of the tumor. If any red fluorescence is observed, the more laser treatment is necessary. The report describes two cases involving men with centrally located early-stage lung cancer for whom this approach was successfully used.
Opening the Airways
Many patients with advanced central lung cancer are confronted with airway obstruction, which interferes with their ability to breathe normally. The obstruction is caused by tumors in the lumen of the bronchial passages. These are typically patients for whom previous treatment with surgery, radiotherapy, and chemotherapy has failed.
For such patients, as described by Chinese oncologists in the December 2013 issue of Photodiagnosis & Photodynamic Therapy, PDT can be performed with laser light delivered through quartz fibers that are passed through a flexible endoscope following intravenous administration of the photosensitizer. After the first light treatment, the endoscopic procedure can be repeated, and necrotic tissues can then be mechanically removed from the lumen. Both the deep original lesions and the newly exposed cancer lesions can then be re-treated, and, if necessary, the areas can be cleaned repeatedly.
This particular PDT strategy was recently tried at the Oncology Department of Nanfang Hospital, Southern Medical University, in Guangzhou, China. The total response rate was about 87%, and the average percentage of airway obstruction due to tumors at different treated sites decreased from 90% to 17%. Also, quality-of-life scores significantly improved after PDT.
In their report, the Chinese researchers offered the following conclusion: “PDT of intractable bronchial lung cancer effectively reduces the amount of lumen obstruction, and improves the patient’s quality of life. PDT may also be an effective palliative treatment, with minor side effects on patients with advanced bronchial lung cancer.”
Keep in mind that these were lung cancer patients for whom no conventional treatment options were deemed viable. Under these circumstances, there is no reason not to consider PDT. Given that lung cancer is generally viewed as a “terminal” disease—that is, a disease with an eventual outcome of death and an overall mortality rate of 98%—investigations of innovative PDT-based treatment combinations to extend or optimize survival are urgently needed.
Support us by buying our book, The Medicine of Light and ebooks from our Photoimmune Discoveries eBook Series.
Sources
Usuda J, Ishizumi T, Inoue T, Takeuchi S, Iijima Y, Ibi T. Photodynamic Diagnosis (PDD) for Central Type Lung Cancers. J Nippon Med Sch. 2013;80(6):402-3.
Cai XJ, Li WM, Zhang LY, Wang XW, Luo RC, Li LB. Photodynamic therapy for intractable bronchial lung cancer. Photodiagnosis Photodyn Ther. 2013 Dec;10(4):672-6
© Copyright 2014, Photoimmune Discoveries, BV