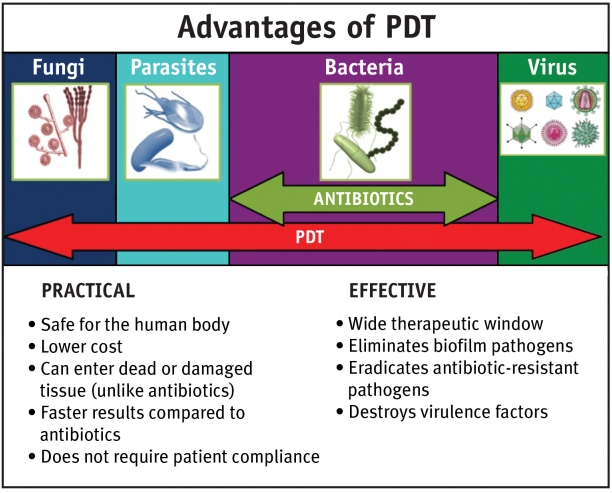
Though photodynamic therapy (PDT) was discovered as an antimicrobial treatment as far back as 1903, it has been mostly used for the treatment of cancer and eye diseases. PDT’s initial promise as an antimicrobial treatment suffered a major setback with the discovery of antibiotics in the 1940s. That discovery revolutionized the treatment of infectious diseases caused by pathogenic microbes (including bacteria, fungi, viruses, and protozoa) and thus numerous antimicrobial medicines became quickly available.
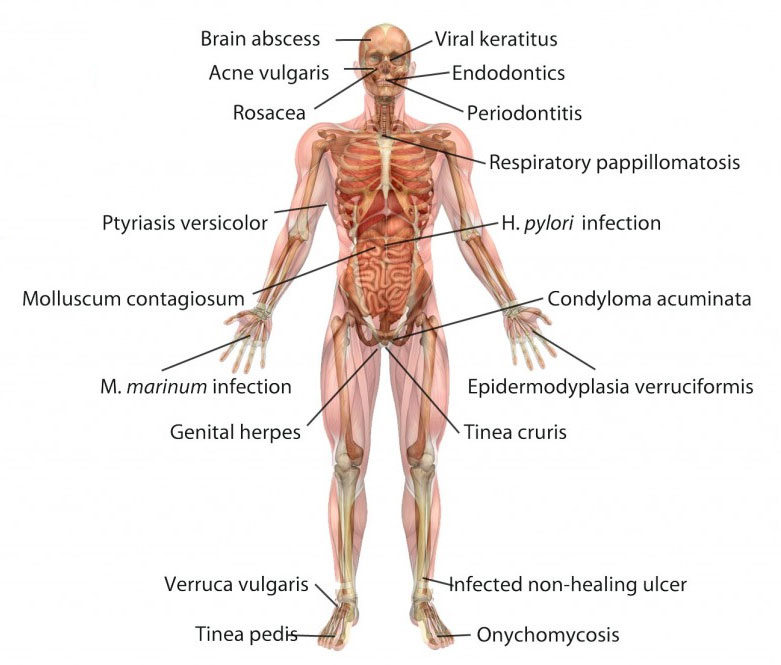
The above illustration depicts the range of human infections that have been clinically treated with PDT. As you can see, antimicrobial PDT has many potential applications. In recent years, this approach has made a strong comeback as a possible way to eliminate multidrug-resistant infections. At the present time, there are no known situations in which microbes have become resistant to antimicrobial PDT despite numerous attempts to induce resistance in laboratory studies.
The idea of using a pill to eliminate the infection seemed vastly simpler and far more attractive on practical grounds to that of a light-based therapy. In the 1970s, studies of antimicrobial PDT resumed and seemed to hold real promise for the treatment of viral infections. Nevertheless, this practice ceased when a paper in the prestigious New England Journal of Medicine claimed that the procedure was largely ineffective. Some doctors also raised the erroneous concern that the use of light could somehow cause cancer.
Thus, despite its discovery over a century ago, progress in the field of antimicrobial PDT has been very gradual. With the steady spread of antibiotic resistance throughout the world, there has been renewed interest in the possibility of using antimicrobial PDT, also known as photodynamic inactivation (PDI). It is understood that antibiotics and other antimicrobial drugs have a very limited future, and that reasonable alternatives are urgently needed.
Support us by buying our book, The Medicine of Light, and ebooks from our Photoimmune Discoveries eBook Series.
Sources
Yin R, Dai T, Avci P, Jorge AE, de Melo WC, et al. Light based anti-infectives: ultraviolet C irradiation, photodynamic therapy, blue light, and beyond. Curr Opin Pharmacol. 2013;13(5):731-62.
Vatansever F, de Melo WC, Avci P, Vecchio D, Sadasivam M, et al. Antimicrobial strategies centered around reactive oxygen species–bactericidal antibiotics, photodynamic therapy, and beyond. FEMS Microbiol Rev. 2013;37(6):955-89.
Sharma SK, Mroz P, Dai T, Huang YY, St Denis TG, Hamblin MR. Photodynamic Therapy for Cancer and for Infections: What Is the Difference? Isr J Chem. 2012;52(8-9):691-705.
Huang YY, Tanaka M, Vecchio D, Garcia-Diaz M, Chang J, et al. Photodynamic therapy induces an immune response against a bacterial pathogen. Expert Rev Clin Immunol. 2012;8(5):479-94.
Vera DM, Haynes MH, Ball AR, Dai T, Astrakas C, et al. Strategies to potentiate antimicrobial photoinactivation by overcoming resistant phenotypes. Photochem Photobiol. 2012;88(3):499-511
Kharkwal GB, Sharma SK, Huang YY, Dai T, Hamblin MR. Photodynamic therapy for infections: clinical applications. Lasers Surg Med. 2011;43(7):755-67.
St Denis TG, Dai T, Izikson L, Astrakas C, Anderson RR, Hamblin MR, Tegos GP. All you need is light: antimicrobial photoinactivation as an evolving and emerging discovery strategy against infectious disease. Virulence. 2011;2(6):509-20.
Dai T, Huang YY, Hamblin MR. Photodynamic therapy for localized infections–state of the art. Photodiagnosis Photodyn Ther. 2009;6(3-4):170-88.
Maisch T. A new strategy to destroy antibiotic resistant microorganisms: antimicrobial photodynamic treatment. Mini Rev Med Chem. 2009;9(8):974-83.